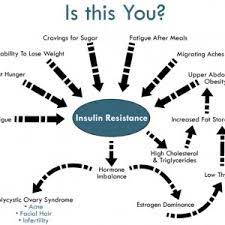
The most common cause of infertility today is polycystic ovary syndrome. PCOS is a metabolic condition in which insulin and testosterone elevations disrupt pituitary feedback loop coordination. Insulin resistance appears to play a major role in the development of PCOS.
What is Polycystic ovary syndrome
The prevalent illness known as a polycystic ovarian syndrome (PCOS) alters how a woman’s ovaries function.
The three main characteristics of PCOS are:
- irregular periods, which indicates that your ovaries don’t release eggs on a regular basis (ovulation)
- Excessive quantities of “masculine” hormones in your body, such as extra facial or body hair, may be caused by excess androgen.
- Polycystic ovaries are larger and contain several fluid-filled sacs (follicles) that surround the eggs (but despite the name, you do not actually have cysts if you have PCOS)
If you have at least 2 of these features, you may be diagnosed with PCOS.
It’s difficult to estimate the precise number of women who have PCOS, but it’s believed to be quite widespread—it affects roughly 1 in 10 women in the UK, and more than half of these women don’t exhibit any symptoms.
Polycystic ovary syndrome signs and symptoms (PCOS)
• irregular or nonexistent periods; difficulties conceiving due to irregular ovulation or failure to ovulate; hirsutism (excessive hair growth), which typically affects the face, chest, back, or buttocks; weight gain; thinning and hair loss from the scalp; oily skin or acne;
Additionally, PCOS is linked to a higher risk of later-life health issues like type 2 diabetes and high cholesterol.
What results in PCOS, or polycystic ovarian syndrome?
Although the exact aetiology is unknown, PCOS frequently runs in families. It has to do with the body’s aberrant hormone levels, which include elevated insulin levels. The hormone insulin regulates the body’s sugar levels.
In order to overcome their body’s resistance to insulin, many women with PCOS create higher quantities of insulin. The production and activity of hormones like testosterone are boosted as a result of this. The quantity of insulin your body generates also increases when you are overweight or fat.
Taking care of polycystic ovarian syndrome (PCOS)
Although there is no known treatment for PCOS, if you believe you may be affected, we can assist you. Most PCOS sufferers can become pregnant with the right therapy.
The benefits of functional medicine for PCOS
From the perspective of functional medicine, there are several things that may be done to naturally increase insulin sensitivity and decrease androgen levels to support the restoration of normal hormonal function:
• A nutrition and exercise plan designed to lower insulin levels and improve insulin sensitivity forms the basis of a PCOS regimen. Additionally, there are a variety of specialised nutrients and herbs that can be used to balance blood sugar levels and control insulin.
• For those who are overweight, achieving a healthy body weight can assist in regulating insulin and hormones. Whereas previous diets may have failed, a customised food plan created just for PCOS can help you lose weight.
To help balance hormone levels and lessen PCOS symptoms and indicators, some herbs, nutrients, and therapeutic foods can be consumed. Which of these is best for you will be determined by your practitioner. Testing that we may use could include:
· Thyroid function test
· Digestive system testing
· Blood testing
· Urine testing
· Saliva Testing
· Heavy Metal testing
· Fatty Acid testing
· Anti-Oxidants
· Minerals and Vitamin Testing
Dr Stavy can prepare a personalised treatment plan for you based on a comprehensive analysis which can include:
· Advice on nutrition
· A plan and advice for exercising
· Medication
· A lifestyle change and recommendations
Diet
Dietary changes have a major impact on PCOS in two areas: weight control and insulin sensitivity and resistance.
However, since insulin has a big part to play in PCOS, one of the best things patients can do to treat the illness is to control their insulin levels using a PCOS diet. Insulin resistance occurs frequently in PCOS patients.
People with PCOS may feel better if they eat a diet that fits their nutritional needs, helps them maintain a healthy weight, and encourages optimal insulin levels.
Three diets that may help people with PCOS manage their symptoms are:
Low glycemic index (GI) diet: this diet causes insulin levels to not rise as much or as soon as other foods, such as some carbohydrates, because the body digests these foods more slowly. Whole grains, legumes, nuts, seeds, fruits, starchy vegetables, and other unprocessed, low-carbohydrate foods are all included in a low GI diet.
An anti-inflammatory diet: Foods like berries, fatty salmon, leafy greens, and extra virgin olive oil that are anti-inflammatory may lessen inflammation-related symptoms like weariness.
The DASH diet: The Dietary Approaches to Stop Hypertension (DASH) diet is frequently advised by medical professionals to lower the risk or effects of heart disease. It might also aid in treating PCOS symptoms. Fish, poultry, fruits, vegetables, whole grains, and low-fat dairy products are abundant in a DASH diet. Foods that are heavy in sugar and saturated fat are discouraged by the diet.
A healthful PCOS diet can also include the following foods:
- natural, unprocessed foods
- high-fibre foods
- fatty fish, including salmon, tuna, sardines, and mackerel
- kale, spinach, and other dark, leafy greens
- dark red fruits, such as red grapes, blueberries, blackberries, and cherries
- broccoli and cauliflower
- dried beans, lentils, and other legumes
- healthful fats, such as olive oil, as well as avocados and coconuts
- nuts, including pine nuts, walnuts, almonds, and pistachios
- dark chocolate in moderation
- spices, such as turmeric and cinnamon
In general, people on a PCOS diet should avoid foods already widely seen as unhealthful. These include:
- Refined carbohydrates, such as mass-produced pastries and white bread.
- Fried foods, such as fast food.
- Sugary beverages, such as sodas and energy drinks.
- Processed meats, such as hot dogs, sausages, and luncheon meats.
- Solid fats, including margarine, shortening, and lard.
- Excess red meat, such as steaks, hamburgers, and pork.
How PCOS affects your body
- Excess testosterone – we all produce some testosterone, but too much can prevent ovulation and change your menstrual cycle.
- Insulin resistance – your body has to produce much more insulin than normal to keep blood sugar levels stable. Excess insulin floating around also increases testosterone production and can lead to…
- Reduced fertility
- Irregular or absent periods
- Excess hair on your body and face (hirsutism)
- Less hair on your head (alopecia)
- Changes in your skin, such as acne or darkened skin patches
As a result of all these physical changes that occur after diagnosis, you can also find that your self-confidence and perception of your body suffer or that you struggle with despair and worry.
There is good news, though! Many of these signs and symptoms can be alleviated with a few lifestyle changes, especially increased activity. The best exercises and their benefits are listed here.
CARDIO
Good for reducing insulin resistance, boosting fertility, stabilising mood
Walking quickly, jogging, cycling, or swimming are all excellent exercises that can benefit PCOS. By increasing your body’s sensitivity to insulin, this kind of exercise lowers your risk of developing type 2 diabetes and cardiovascular disease. A daily workout of at least 30 minutes can help with weight control, anxiety and depressive symptoms, menstrual cycle regularity, and ovulation. Additionally, regular modest exercise can improve your chances of getting pregnant if you’re going to begin IVF.
STRENGTH TRAINING
Good for reducing insulin resistance, increasing metabolic rate, and improving body composition (more muscle and less fat tissue)
Squats, push-ups, and tricep dips are bodyweight activities that enhance insulin function while simultaneously increasing muscle mass, which increases metabolism. But don’t worry, unless you’re using steroids, you won’t bulk up. Simply put, having more muscle means burning more calories during exercise as well as all day long, even when at rest. The greatest method to ensure you’re developing a lean body, achieving a healthy BMI, and lowering your risk of chronic diseases like type 2 diabetes is to combine resistance exercises with cardio workouts.
HIGH-INTENSITY INTERVAL TRAINING
Good for increasing cardiovascular fitness and decreasing waist circumference
Short bursts of intense labour are alternated with recoveries of lesser intensity throughout intervals. It’s a quick approach to improving your cardiovascular fitness and has additional PCOS benefits. A vigorous spin bike workout burns tons of calories and gets rid of belly fat more quickly than, say, a brisk walk. This can assist you in losing 5 to 10 per cent of your body weight, which, according to studies, can lessen the symptoms of PCOS by lowering excessive testosterone levels and enhancing insulin sensitivity.
CORE STRENGTH
Good for general well-being and injury prevention, preparing your body for pregnancy
Include core training in your regimen because being overweight can lead to lower back pain and bad posture. Knowing how to activate these muscles will help you avoid exercising-related injuries. They support the spine. Start strengthening your pelvic floor muscles if you’re attempting to get pregnant as well! These muscles, which are also a component of your core, assist a healthy pregnancy by preventing incontinence, enhancing sexual health, and enhancing pelvic stability.
Pick an activity you enjoy doing because that is the exercise that will be most effective for you!
Supplements
PCOS supplements are becoming a more popular way to treat PCOS symptoms (which often include hair loss, weight gain, acne, insulin resistance, and irregular periods, to name a few). But when you’re faced with the hundreds of options available at the pharmacy and have no idea which PCOS supplements can actually improve your health, this answer can quickly appear overwhelming. So where should you begin? Which PCOS supplements specifically have scientific backing to assist treat this hormonal imbalance? And ultimately, which ones will be the most beneficial to your body and you?
- Inositol
Inositols like myo- and d-chiro inositol B-vitamins (which should be combined in a 40:1 ratio), are a type of carbocyclic sugar naturally found in foods like fruits, beans, nuts, animal foods, and grains, and they offer antioxidant properties.
- Vitamin D
Supplementation of vitamin D in women with PCOS improves menstrual regularity (after 3 months of supplementation), while it also has been shown to improve fertility and pregnancy rates during assisted reproduction therapy. If these results aren’t enough, vitamin D supplementation has also been shown to improve mood and reduce likelihood of depression in women both with and without PCOS!
- B Complex
B vitamins such as B12 and folate are among the most helpful in treating PCOS naturally. Specifically, they’re thought to help fight insulin resistance in those with PCOS.
- Omega 3
Omega 3s are so powerful thanks to their anti-inflammatory properties, especially when it comes to treating inflammatory and autoimmune conditions.
- Berberine
Berberine is an alkaloid extracted from herbs, and it can be taken in liquid or capsule form. When it comes to naturally treating PCOS, it’s particularly noteworthy for its role in improving insulin resistance through better insulin signal transduction.
- Magnesium
Did you know that whether you’re considered a healthy weight, overweight, or obese on a BMI scale, that if you have PCOS, there’s a high chance you have insulin resistance?
- Zinc
Zinc is a critical micro element that is responsible for the regulation of cell growth, hormone release, reproduction, and immunological response.
For more information or if you would like to discuss treatment and management for hypothyroidism with Dr Stavy, then please contact us via email: info@drstavy.com.